Research Programme
Research Programme
Improving the quality and humanity of hospital care for people living with dementia
Funded by
The number of people living with dementia now being cared for within our hospitals is increasing. People living with dementia represent 77% of patients arriving at our hospitals with urgent unscheduled care needs; and are estimated to occupy at least one in four acute hospital beds (Alzheimer’s Society 2009, 2016), the equivalent of 3.2 million bed days per year.
These figures are considered to underestimate the volume of admissions, with the number closer to one in two beds including people whose dementia is still undiagnosed. Some hospitals report this patient group represents as many as half of their acute admissions (Alzheimer’s Society 2016).
There has been increasing recognition that action is required now to improve the experience and outcomes of the increasing numbers of people living with dementia admitted to hospital.
A large number of government inquiries and reports have identified wide-spread poor dementia care in hospitals, with wide variations in quality. This variation means that people living with dementia will experience poor care at some point in their care pathway through the hospital.
Almost all people living with dementia will have at least one unscheduled hospital admission following their diagnosis, however, once admitted they become highly vulnerable.
People living with dementia are at significantly higher risk of delayed discharge and are likely to experience some form of functional physical or cognitive decline during their admission (Mukadam and Sampson 2011).
One in four people living with dementia will die during their hospital admission, with a third declining to such an extent over the course of an admission that they are not able to return home and live independently. This means moving into long term supported care, breaking up families, homes and care networks.
Dementia is the only condition in the top 10 causes of death in the UK without a treatment to prevent, cure or slow its progression. The work of biomedical science and the research investment in this is critical to changing this and improving quality of life.
However, we cannot wait for this, we need significant investment in research, in training and education, to support our hospitals to deliver evidence based high quality care to ensure people (and their families) can live well with dementia now, and that hospitals are a site of treatment, recovery and re-enablement when people living with dementia require them.
In response, our research provides foundational understandings of the organisation and delivery of care within the contemporary hospital and its impacts on both patients living with dementia and ward staff. Applying ethnography and sociological theory to providing new knowledge and theoretical developments in understandings of the cultures, organization and delivery of hospital care.
Research Studies
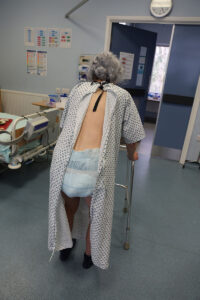
Facilitating Continence
Facilitating continence in people living with dementia in acute ward settings: what the evidence says
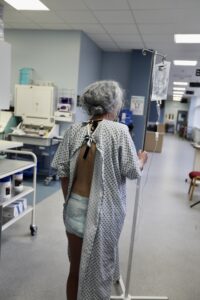
Dementia & Continence
Understanding how to facilitate continence for people with dementia in acute hospital settings: raising awareness and improving care.

Restrictive Practices Study
Understanding the everyday use of restrictive practices in the care of people living with dementia during a hospital admission: reducing inappropriate use, identifying good practice and alternative approaches to reduce risk and improve care.

Resistance Study
Underserved and overlooked: Investigating the management of refusal of care in people with dementia admitted to hospital with an acute condition.
Our Programme
- Provides the foundational knowledge examining the everyday organisation and delivery of care for people living with dementia in acute hospital wards.
- Uses this to develop evidence based low-cost interventions to inform changes that may lead to shorter acute hospital stays, more effective and humane management and care; all factors that mitigate suffering in patients and support ward staff.
- Develops and delivers innovative evidence-based open access learning to support and educate staff working with people living with dementia.
- Challenges social inequalities by working in collaboration with people living with dementia, their families, and ward staff to increase inclusion, identify priorities, and to shape contemporary care debates.
- Collaborates with filmmakers, BBC documentary teams, news media, and the arts, to develop and deliver a programme of knowledge transfer to inform public discourse, public policy and NHS practice.